
The Alzheimer’s Association recently released their annual “Facts and Figures” report. It’s always a sobering collection of data, but important to document and share to increase Alzheimer’s awareness and to ensure the disease remains a high priority for funding research and care support initiatives.
Here’s a roundup of the top Alzheimer’s insights from the report:
- More than 7 million Americans are living with Alzheimer’s.
- 1 in 3 older adults dies with Alzheimer’s or another dementia.
- Approximately 1 in 9 people age 65 or older has Alzheimer’s.
- Women account for 2/3 of Alzheimer’s cases in America.
- Race plays a role in Alzheimer’s risk, with Black Americans (twice as likely) and Hispanic Americans (1.5 times as likely) to develop the disease vs White Americans.
- Those with Alzheimer’s or other dementias have twice as many hospital stays and more skilled nursing facility stays and home health care visits per year than other older people.
- The lifetime cost of care for a person living with dementia is estimated at a whopping $405,262 (in 2024 dollars.) What’s worse is that 70 percent of those costs are borne by family caregivers.
The report also highlights the growing contributions of family caregivers.
- Nearly 13 million Americans provide unpaid care for people with Alzheimer’s or other dementias.
- About 30% of caregivers are age 65 or older.
- Most caregivers (66%) live with the person with dementia in the community.
- Approximately 25% of dementia caregivers are “sandwich generation” caregivers, juggling the care demands of an aging parent and at least one child.
- Caregivers are stressed out: Nearly 60 percent of dementia caregivers report feeling high to very high emotional stress.
- Unpaid caregivers provided more than 19 billion hours of care valued at more than $446 billion.
- Forty-one percent of caregivers have a household income of $50,000 or less.
Below is a video synopsis of the report’s most important findings.
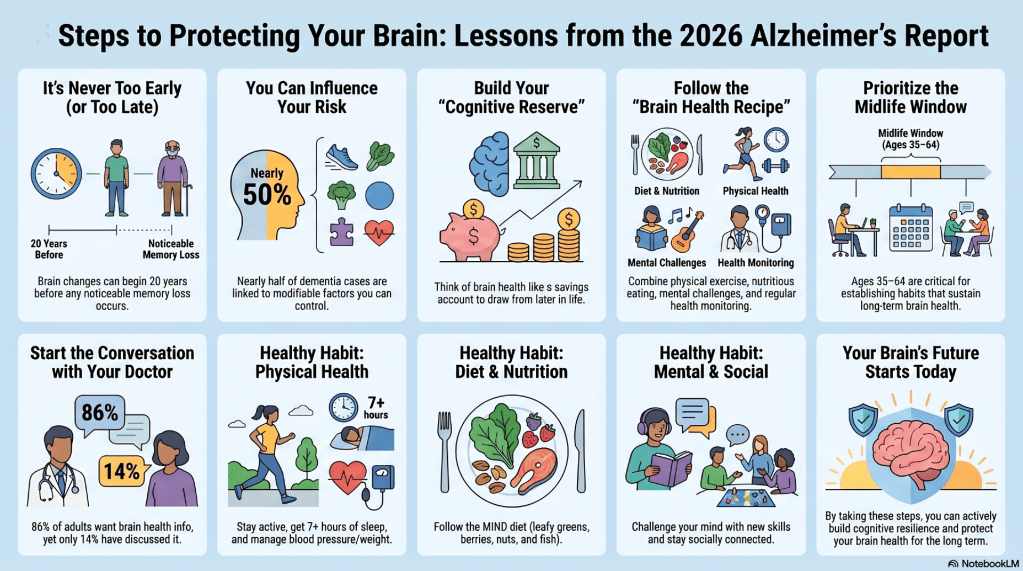
Based on the Alzheimer’s Association report and resources, I used NotebookLM to create an infographic of ways to protect the brain, which appears at the top of this blog post. This year’s report found that Americans have a deep interest in brain health and understand that lifestyle choices can have an impact but are unclear about how to implement them in their own lives. The good news is that supporting brain health isn’t that complex: moderate exercise, decent diet, managing stress, good sleep quality, engaging in brain-friendly hobbies like puzzles, learning new languages, or playing a musical instrument. The tough part is being consistent in implementing these healthy lifestyle choices. Every positive choice helps, so consult with your doctor to see which lifestyle change may be most beneficial for you.














![Pageflex Persona [document: PRS0000038_00069]](https://memoriesproject.files.wordpress.com/2014/02/reluctant-caregiver-cover.jpg)






